Tel Aviv University’s cyborg cardiac patch could replace transplants
Researchers are currently examining how his proof of concept could apply to the brain and spinal cord to treat neurological conditions.
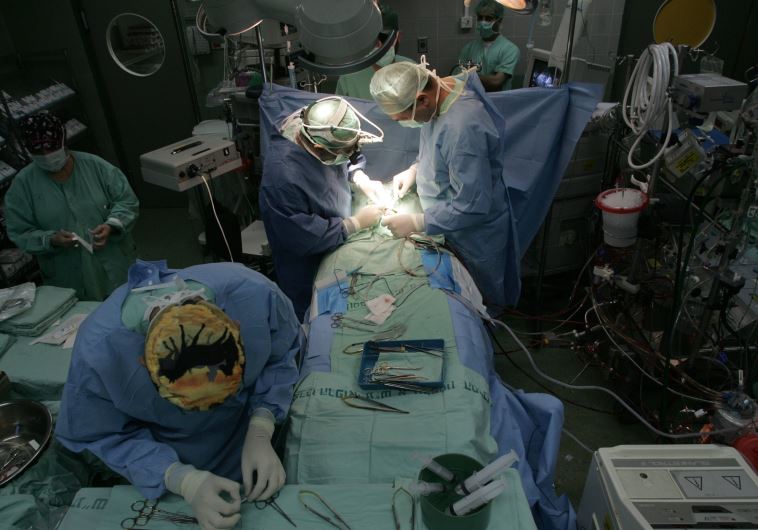 Israeli doctors perform heart surgery on a baby from Gaza, at Wolfson Hospital near Tel Aviv Updated:
Israeli doctors perform heart surgery on a baby from Gaza, at Wolfson Hospital near Tel Aviv Updated: