Israeli, Palestinian and American collaboration saves life of Nablus teen
17-year-old girl from West Bank city had been suffering from serious and rare endocrine disorder that led PA doctors to refer her to Israeli hospital.
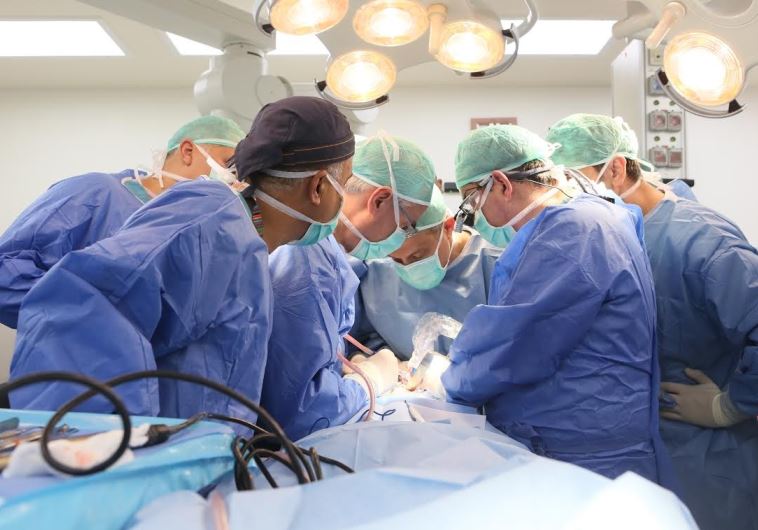 Israeli, Palestinian and American surgery collaboration saves life of Nablus teen(photo credit: COURTESY RAMBAM MEDICAL CENTER/DR. OMRI EMODI)Updated:
Israeli, Palestinian and American surgery collaboration saves life of Nablus teen(photo credit: COURTESY RAMBAM MEDICAL CENTER/DR. OMRI EMODI)Updated: