4,000 Israelis a year die from resistant superbugs
Antibiotic resistance happens when bacteria change and become resistant to the antibiotics used to treat the infections they cause.
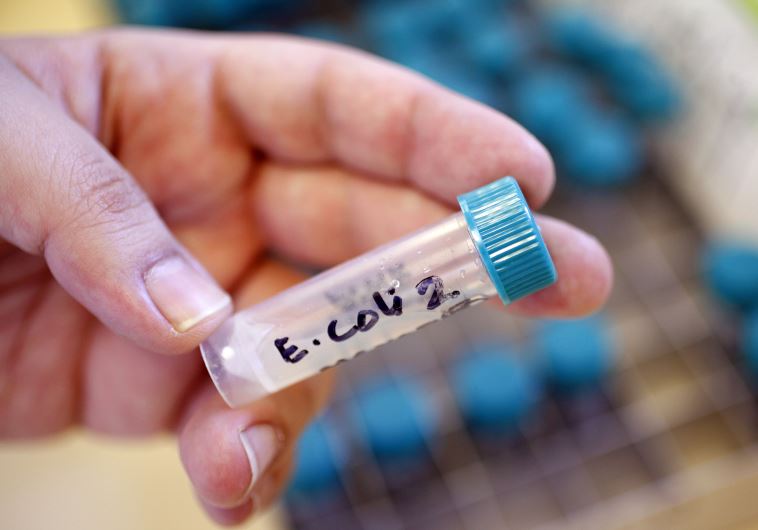 A sample bottle containing E. coli bacteria is seen at the Health Protection Agency in north London
A sample bottle containing E. coli bacteria is seen at the Health Protection Agency in north London