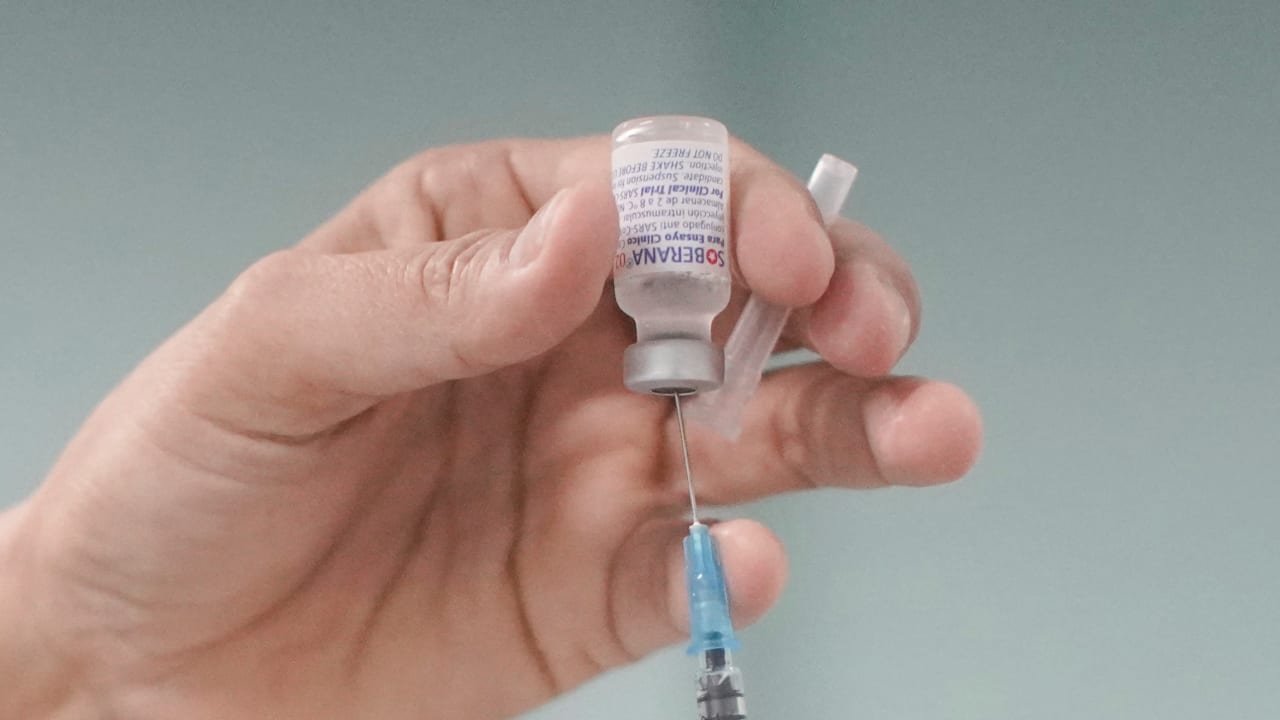
Israel hopes to someday open a vaccine manufacturing plant. How feasible is this, and would it allow Israel to keep up with global powers in pandemic prevention?
Last November, it was reported that Israel was eyeing the idea of setting up its own vaccine production facility. That would give it the independent capability to take countermeasures for any future pandemic threats, coronavirus related or not.
At the time, the Finance Ministry announced an approach to market (AtM), offering the public the opportunity to step forward with business proposals and information for the purpose of “examining, commercially and practically, a possible framework for establishing a vaccine manufacturing facility in Israel that shall have independent abilities for manufacturing vaccines on a routine basis, as well as the capability to manufacture vaccines for future pandemics.”
According to the most recent update published, the deadline for submissions has been extended until March 17. It is likely that no further information on the project will be available until then.
But what is involved in opening up an independent vaccine manufacturing plant? What would this mean for Israel in terms of the approach to COVID-19 and any future pandemics or epidemics?
A declaration of independence
First, Israel is currently completely dependent on imported vaccines to fight any pandemic or epidemic. This means that should something happen to the vaccines in transit, or if the shipment is delayed for any reason, the country could face a vaccine shortage and be unable to inoculate the public in a safe and timely manner.
One only needs to look at recent history to see the reality of this play out, albeit not in Israel. In January 2021, Canada fell far behind its COVID-19 vaccination targets due to a production delay at the Pfizer factory in Belgium, leading to zero new shipments arriving in the country.
Countries such as the US and the UK, however, which had their own production capacity, did not experience the same delays.
Independent vaccine production would allow Israel to set and meet targets without relying on outside assistance that may or may not arrive as needed.
However, the delivery of vaccines and the inoculation of the public are the last stages in the vaccine-making process. And while an independent manufacturing plant in Israel could increase the speed at that late stage, what other challenges could be faced beforehand?
<br>The cost of homegrown vaccines
Establishing a vaccine manufacturing facility that meets the goals laid out by the AtM is not as simple as some may hope. A facility can cost anywhere between $50 million to $700m. to build, and the process can take three or more years. Then there are the added costs of raw materials and other consumables, utilities, personnel and quality-assurance controls.
The cost alone may be a reason to make some countries think twice before opening such a facility. But should this be a deterrent for Israel?
While the exact price Israel paid to receive the millions of Pfizer coronavirus vaccines in early 2021 – and again at later dates – has not been released to the public, it is understood that a significant sum was paid to acquire as many vaccines as the country did in the time it did. This would imply that receiving vaccines in a timely manner is important to Israel, and the monetary cost required to do so is a small price to pay.
How will Israel be able to produce vaccines under time pressure?
According to Vaccines Europe, a specialized vaccines group within the European Federation of Pharmaceutical Industries and Associations, it takes 12-36 months to manufacture a vaccine before it is ready for distribution. Of this time period, 70% is dedicated to quality controls, ensuring that the vaccines are safe for public use and work as intended.
Any future manufacturing facility, the Finance Ministry AtM said, must have “the ability to confront familiar and unfamiliar pathogens, including pathogens causing a pandemic.”
The only way Israel would be able to achieve a fast response to unfamiliar pathogens as required would be if the necessary equipment was already in place to produce a wide array of vaccines, which could then be adjusted as needed.
Addressing this issue specifically, the AtM said: “Israel’s facility must have the ability to use a diversity of vaccine technologies, such as viral vectors, inactivated vaccines, live attenuated vaccines, proteins and nucleic acid,” as well as “the ability for fast conversion or other versatility in the manufacturing process, considering the multiple technologies that exist in the market and the range of potential pathogens.”
THERE IS no such thing as one size fits all when it comes to vaccine production. While some vaccines contain a dead virus or a small amount of virus protein to trigger an immune response in the body, others contain genetic material from the virus that the body then turns into virus proteins that it uses to produce antibodies.
The AtM would require the vaccine-manufacturing plant to be able to produce a number of vaccines, all using vastly different methods, meaning they must have the facilities to produce different vaccines at the same time.
For example, the AtM specifies the need for a facility that can create both viral vector vaccines, which use a modified version of the virus that does not cause disease to stimulate an immune response, and attenuated vaccines that reduce the virulence of a pathogen while still keeping it alive, allowing the body to create an immune response in a harmless way.
If the facility is producing this wide variety of vaccines on a regular basis at a consistent level, the preparation time needed to adjust the vaccines as necessary when a new pathogen becomes a threat will be considerably shorter than if the production of the vaccines only starts after the event.
100 days from demand to distribution
Last June, a report was presented at the G7 Summit titled “100 Days Mission to Respond to Future Pandemic Threats.” It examined the response to COVID-19 across the world and used it as a basis to build a plan for any future pandemics, ensuring that they would be met with a quicker, more efficient response than the world was able to produce during the coronavirus pandemic.
Whereas the first coronavirus vaccine was not cleared for emergency use by the World Health Organization until 336 days after a public health emergency was declared, the plan outlined in the G7 report would see vaccines ready to be produced on a large scale by the 100th day after the declaration of such an emergency.
The plan would be split into two parts: preparation for a pandemic and acting during a pandemic.
In the first part of the plan, vaccine-manufacturing companies must embed the best working practices into their daily routines, including the establishment of an international network of clinical trials with effective data sharing, better regulation and the sharing of knowledge through transferable manufacturing processes.
Then, with all the background work done ahead of time, should another pathogen begin to spread in a way that causes concern, manufacturing plants would shift to work under the second part of the plan to meet the 100-day deadline.
This would see them prioritize their work to focus on the specific pandemic pathogen, refocusing clinical trials to engineer a working vaccine, enabling speed of production and distribution.
The report said both industry and academia should focus on priority pathogens, which include respiratory viruses, coronaviruses and influenza.
“For instance, preparing a pan-coronavirus vaccine or antibody therapies that can be adjusted if a deadly form of coronavirus appears again,” it said. “Similarly, we should embed simplified transferable vaccine manufacturing processes as the norm.”
In short, highlighting the pathogens most likely to be a threat, and staying alert to new threats at all times, will allow for quicker vaccine production, as the materials will already be prepared and will only need to be adjusted as appropriate, shortening the wait time considerably.
Although Israel is not part of the G7, it is clear that the Finance Ministry, along with the other government bodies involved in producing the AtM, envisions a similar road map for the country’s future health emergency preparation and response.
“We don’t know when or from where the next threat will emerge, so we need to work together, between sectors and across national borders, to make the exceptional the everyday. The 100 Days Mission is ambitious but achievable and essential,” Sir Patrick Vallance and Melinda French Gates wrote in the foreword to the G7 report.
While Israel is still at least several years away from reaching the goal of independent vaccine production and is only in the earliest of initial stages of preparation, it seems to be clear from the government’s outline that it is following these same principles, albeit on a smaller scale.
Whether the project comes to fruition and, if so, be followed through to completion, remains to be seen. What is clear, however, is that the government does not intend to lag behind the world powers in responding quickly and effectively to any future public health emergencies.