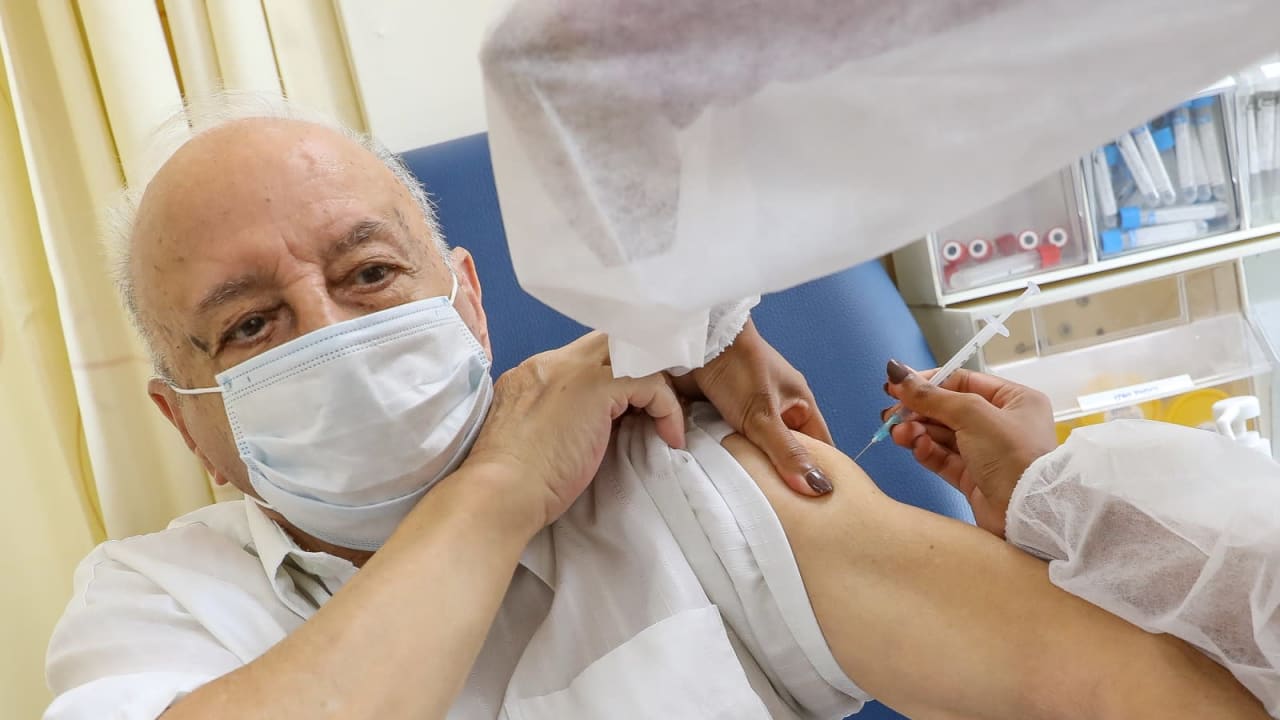
The Health Ministry and other bodies involved in encouraging the public to get vaccinated against COVID-19 and other potentially fatal diseases must “reframe” its messages and “tailor” them to persuade the public, according to researchers at Bar-Ilan University (BIU) in Ramat Gan.
COVID-19 vaccines have saved the lives of tens of millions of people around the world. But while their production could have brought an end to the pandemic had everyone been vaccinated, this outcome was hampered at critical stages by “vaccine hesitancy,” defined by the World Health Organization (WHO) as “the reluctance or refusal to vaccinate despite the availability of vaccines.”
What is the "Nocebo effect?"
This “nocebo effect” – when negative expectations of the patient regarding a treatment cause the treatment to have a more negative effect than it otherwise would have – calls for reframing and tailoring public health messaging.
For example, when a patient anticipates a side effect of a medication, they can experience that effect even if the “medication” is actually an inert substance. The effect is also said to occur in someone who falls ill owing to the erroneous belief that they were exposed to a toxin or to a physical phenomenon they believe is harmful, such as electromagnetic radiation. This is different from the better-known placebo effect, when positive expectations improve an outcome.
Even before COVID-19, the WHO considered vaccine hesitancy to be one of the 10 greatest global threats to public health. The issue has become even more critical in the context of COVID-19. Vaccine hesitancy often results in vaccinations being taken after weighing the pros and cons. It is different from an anti-vaccine position, which usually leads to vaccine refusal and is motivated in large part by ideological, political or religious reasons. Both vaccine hesitancy and anti-vaccination positions are fueled by inaccurate or exaggerated reports of vaccine side effects.
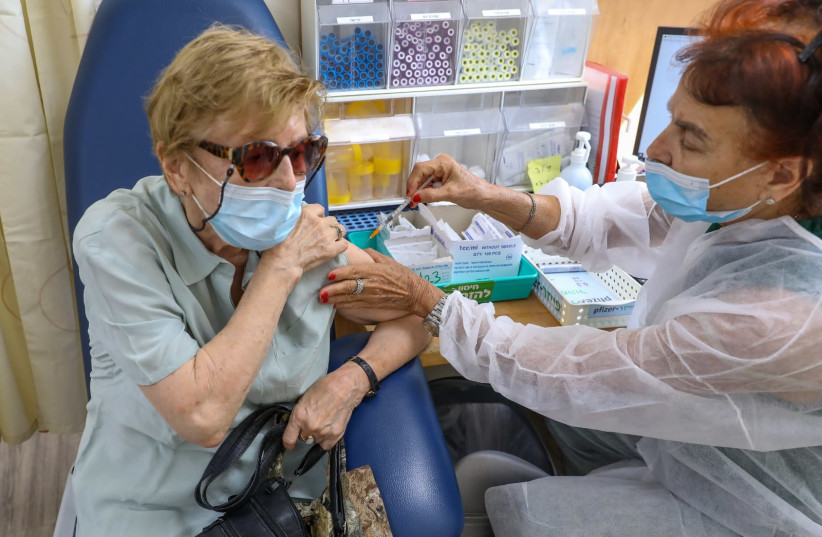
The precise relationship between vaccine hesitancy and COVID-19 vaccination side effects has not previously been explored among vaccinated persons. A fundamental question arises in regard to the directionality of this hesitancy/side-effect link, namely, which variable predicts which. One possibility is that side effects from an earlier dose predict one’s vaccine hesitancy toward a later dose.
Alternatively, one’s psychological negativity (hesitancy) toward an earlier dose could predict subsequent side effects from a later one. The latter direction reflects a nocebo effect, in which side effects are driven by psychological factors rather than by an active treatment component.
The unique, contiguous waves of COVID-19 vaccinations have presented a rare opportunity to test the nocebo effect on vaccinated individuals. In a new study, researchers from BIU and Ariel University examined this issue in 750 older adults. This cohort is a suitable group to test, since they have a high vaccination rate coupled with low side effects, rendering detection of such nocebo effects more challenging.
To address this issue, both variables (vaccine hesitancy and side effects) need to be assessed at two different time points (after the second vaccination dose and six months later after the booster dose) and examine if wave-1 side effects predict wave-2 hesitancy, or whether wave-1 hesitancy predicts wave-2 side effects.
This design is very conservative, and the statistical threshold for such effects is conceptually high, as they have to be maintained beyond all other effects. Results showed only the latter direction to be true. Namely, only earlier vaccine hesitancy toward the second COVID-19 dose predicted subsequent nocebo side effects following the booster vaccination.
“Nocebo components are indicated revealed by vaccine hesitancy prospectively predicting COVID 19 vaccine side-effect.”
Professor Yaakov Hoffman, Bar Ilan University
To put this into perspective, up to 16% of one’s vaccine side effects were explained by earlier vaccine hesitancy. Supplementary analyses revealed that these results held beyond specific side effects and vaccine-hesitancy items.
TYPICAL OF nocebo effects, compatible gender differences were observed. For example, the nocebo effect in females is more impacted by previous experience. The link between previous side effects and current ones was twice as large in females as it was in males.
Beyond the theoretical importance of demonstrating a mind-over-matter effect, these data are novel in additional aspects.
First, they provide a precise (even if underestimated) magnitude of the nocebo effect in vaccinated persons. This is not trivial, as other methods of estimating such nocebo effects typically rely on a statistical assumption that has been challenged, namely, that such effects are additive (constant in treatment groups and non-treatment groups).
Second, public health messaging is typically geared toward unvaccinated persons, stressing that the vaccine is safe. Such public health messaging may be less suited to those who received a vaccination dose and have chosen to discontinue vaccination.
In the United States, there are over 150 million such subsequent refusers, commented Prof. Yaakov Hoffman from BIU’s Interdisciplinary Department of Social Sciences, who was the lead author of a study just published in the journal Scientific Reports under the title “Nocebo components are indicated revealed by vaccine hesitancy prospectively predicting COVID 19 vaccine side-effect.”
Co-author Prof. Menachem Ben-Ezra of Ariel University added, “For such persons, messaging focused on general vaccination safety may be less applicable to partially-vaccinated individuals who have first-hand experience with vaccine side effects and electively chose to discontinue vaccination. Rather, differentiated public health messaging is required.”
The study reveals different risk levels, to which different types of messaging may be tailored. For instance, low-risk individuals (such as older adults and males with low vaccine hesitancy) may benefit from messaging highlighting that for “them,” the vaccine is even safer than for the general public. Yet for those at high risk (younger adults, females, high hesitancy), a public health message focusing on the notion that a significant portion of their side effects doesn’t stem from the treatment (vaccine) may be more beneficial.
Publicizing the fact that COVID-19 vaccine side effects may be driven by anxiety or a previous negative expectation may be extremely effective, they wrote.
“Such messaging should be coupled with nocebo education conveying that these experienced side effects are just as physically real, yet may not stem from treatment but from other factors. The current results, indicating that vaccination side effects comprise nocebo effects, seem to be an important factor that can effectively facilitate public health messaging if it is conveyed in an accepting, humane and non-paternalistic manner,” they said.
“Such messaging should reduce the nocebo effect, and in turn lower vaccination side effects.”
The researchers suggest that this would not only reduce one’s suffering from side effects but also impact the macro level, because if side effects are reduced, there will be less support for overall anti-vaccine campaigns.
These findings may bear on other shots that aren’t given in contiguous waves and thus cannot be examined in the above fashion.
Hoffman concluded, “Most importantly, as COVID-19 may still be a threat, and vaccines are still offered, public health messaging should consider addressing the issue that side-effects comprise a nocebo component.”