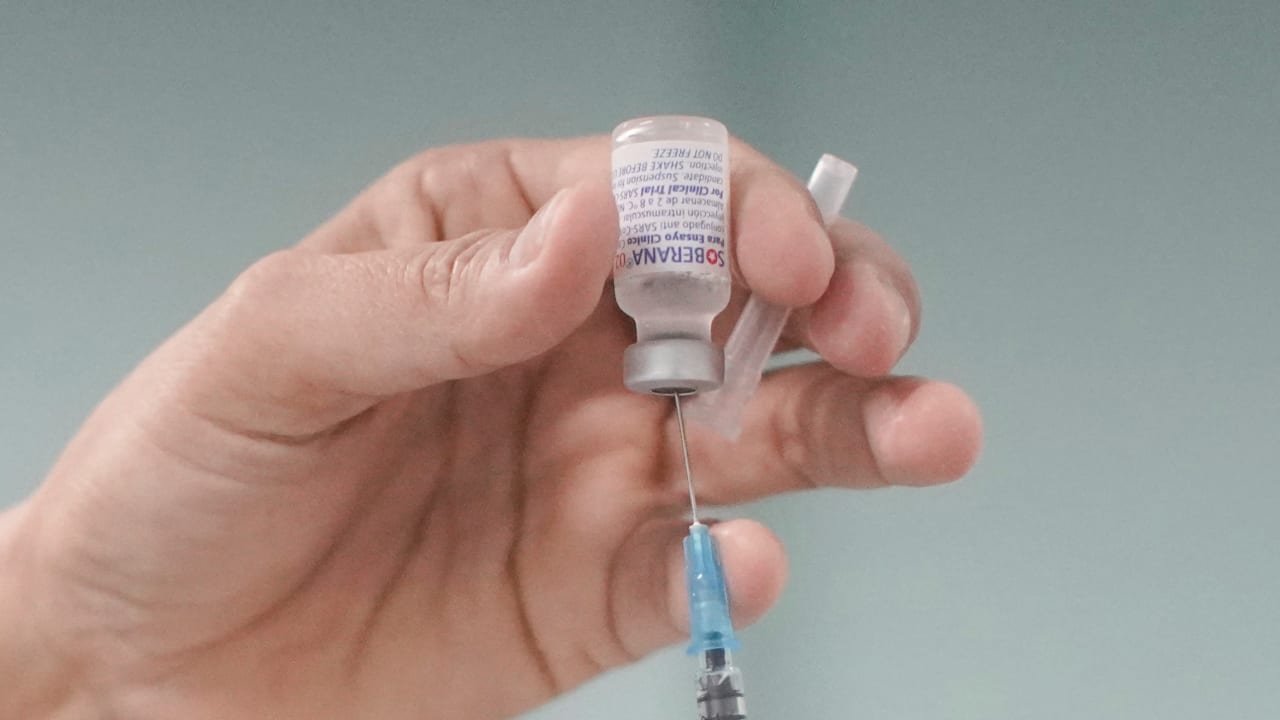
The panel advising the Health Ministry on the corona pandemic will discuss the possibility of giving a fourth vaccine to immunocompromised patients, The Jerusalem Post confirmed on Sunday.
In previous months, several studies showed that certain categories of patients with a weakened immune system, such as transplant recipients, were much less likely to develop antibodies after two doses than the general population.
While research showed that the booster generally improved the situation, this was not true for all immunosuppressed individuals.
For example, a study by the Rabin Medical Center-Beilinson Campus in Petah Tikva and Clalit Health Services in August showed that among lung-transplant recipients, 33% developed antibodies after the booster, compared with 18% after the first two shots.
For heart-transplant recipients, the rates were 58% after the third shot and 31% after the second. Among liver-transplant recipients, 71% developed antibodies after the third shot, compared with 47% after the second.

The advisory panel is due to discuss the option for a fourth vaccine later this week.
According to Prof. Cyrille Cohen, head of the immunology lab at Bar-Ilan University, the move makes sense.
“We know that three shots are needed by people with a functional immune system,” Cohen said. “Immunosuppressed patients got their third vaccine already almost six months ago, so it is not a bad idea to offer them another booster, since they are at high risk.”
According to the scientist, it is hard to know if it is going to help.
“It is very complex to answer the question without actually carrying out the procedure,” he said. “We saw how with the third vaccine many were skeptical as Israel started to administer it, and now most of the world agrees that it is needed.”
The crucial element to consider is whether a fourth shot would be safe. According to Cohen, since most side effects associated with the Pfizer vaccine are somehow connected to an overreaction of the immune system, then the additional shot should not be an issue for patients whose system does not react strongly enough.
“Most side-effects we have seen are associated with inflammation or autoimmune syndromes, so it is less likely that these patients develop them,” he said.
The professor also noted that as it happened with the third vaccine, not all immunosuppressed patients should be considered in the same way.
“There is a difference between, for example, transplant recipients, whose immune system is weakened on purpose, and cancer patients, whose immune systems become sometimes weakened as a side effect of treatment,” Cohen said.
In July, the Health Ministry started to administer booster shots to specific categories of patients.
For example, cancer patients suffering from solid tumors such as breast, lung or colon cancer did not qualify, while people with rheumatological or autoimmune diseases being treated with specific drugs, and those with certain hematologic malignancies and heart, lung, kidney or liver transplant recipients, did qualify, according to the ministry.
Asked if the idea of a fourth vaccine could weaken the public’s trust in vaccination, Cohen said it was important to remember that not all vaccines are the same, and it is not unusual for some of them to be administered on a regular basis.
“There are some vaccines that are very efficient, like the ones against childhood diseases,” he said. “There are others that are good to prevent severe diseases but not so effective to prevent infection. There are vaccines that need to be administered every year, like the one against the flu.
“I think that eventually, a mix between vaccines and natural exposure will help us make the coronavirus less threatening,” Cohen said. “At the moment, vaccines are the best way to fight the pandemic, and we have to be grateful for that.”