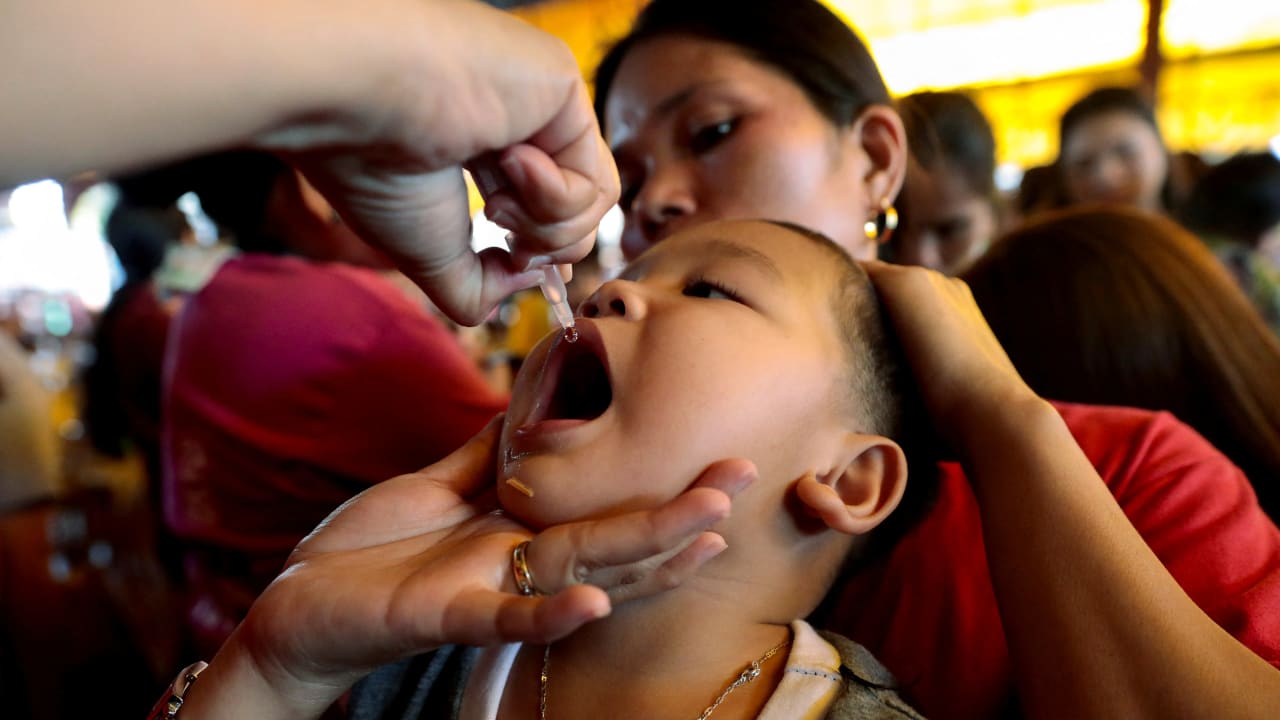
The outbreak of polio virus has largely been overcome and is under control, said Dr. Sharon Alroy-Preis, the Health Ministry’s public health chief at an online briefing for health journalists on Thursday. As a result, the health funds will no longer invite children and teens between the ages of seven and 17 to come in with parents for two drops of oral polio vaccine (OPV).
No polio virus has been found in the country’s sewage in the last month, she reported, but the ministry will only be able to say the outbreak is over if this situation continues for five more months and no child beyond the Jerusalem girl who was paralyzed – and is now undergoing rehabilitation – contracts the clinical disease.
The ministry instructed Tipat Halav infant clinics to give the first polio shot (inactivated polio vaccine, or IPV) at six weeks instead of two months to protect newborns, followed by OPV at 10 weeks. The well-baby clinics have reached a 99% success rate in injecting newborns with the vaccine, Alroy-Preis continued, and an 85% success rate in giving OPV to babies.
The first case of paralysis and seven more cases of infection without paralysis were in Jerusalem, but then infections without paralysis appeared in Bnei Brak, Tiberias, Modi’in Illit and other places with a large concentration of ultra-Orthodox (haredi) Jews.
“It looks like the outbreak is under control. The ministry is very happy. We had expanded the recommended age of OPV to 17-year-olds who should have been vaccinated at a younger age but weren’t. Their risk of infecting and being infected was lower.”
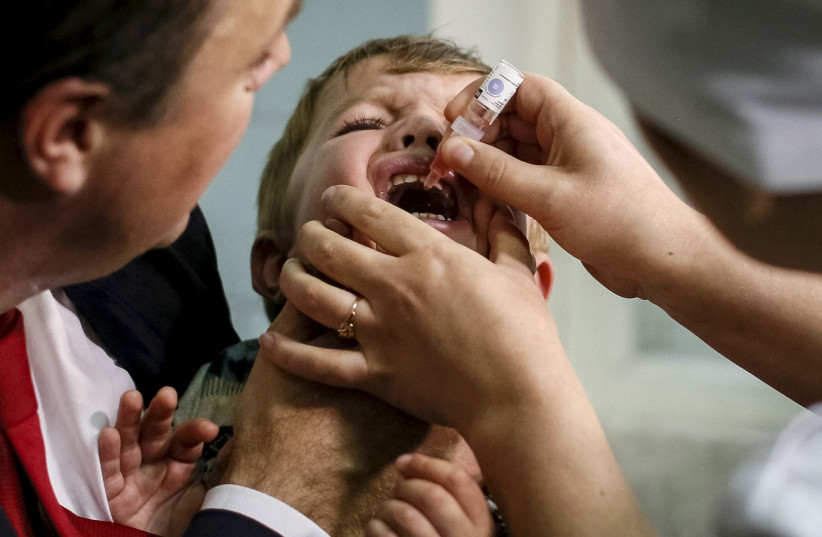
The future of polio vaccination
The ministry will continue its OPV vaccination efforts in Jerusalem and its information campaign, “but in the rest of the country we will give oral vaccine only up to the age of six. If parents, however, made an appointment for children older than six to get the drops, they should go.”
Alroy-Preis added that “the World Health Organization, which supervises and monitors the giving of polio vaccine globally, has praised Israel and its public health experts for acting quickly and efficiently to stop the outbreak. We are watching the situation and checking the sewage all the time, and if it appears again, we will change our policy.”
She conceded that the nationwide campaign to bring teens in for the drops began slowly, but “now there is no need. They are at much lower risk. We are focusing on the younger children. There were no logistic problems, even though health fund clinics are not used to giving polio vaccines unless they also provide Tipat Halav services. In other countries with a polio outbreak, there is usually more than one case of paralysis.”
The inactivated (IPV) vaccine was reintroduced to Israel as an extra line of defense when there was an outbreak in 2013. While the killed vaccine protects recipients against disease if they encounter the virus, the attenuated vaccine – given as oral drops – stops them from spreading the virus, and is therefore seen as a tool for community protection.