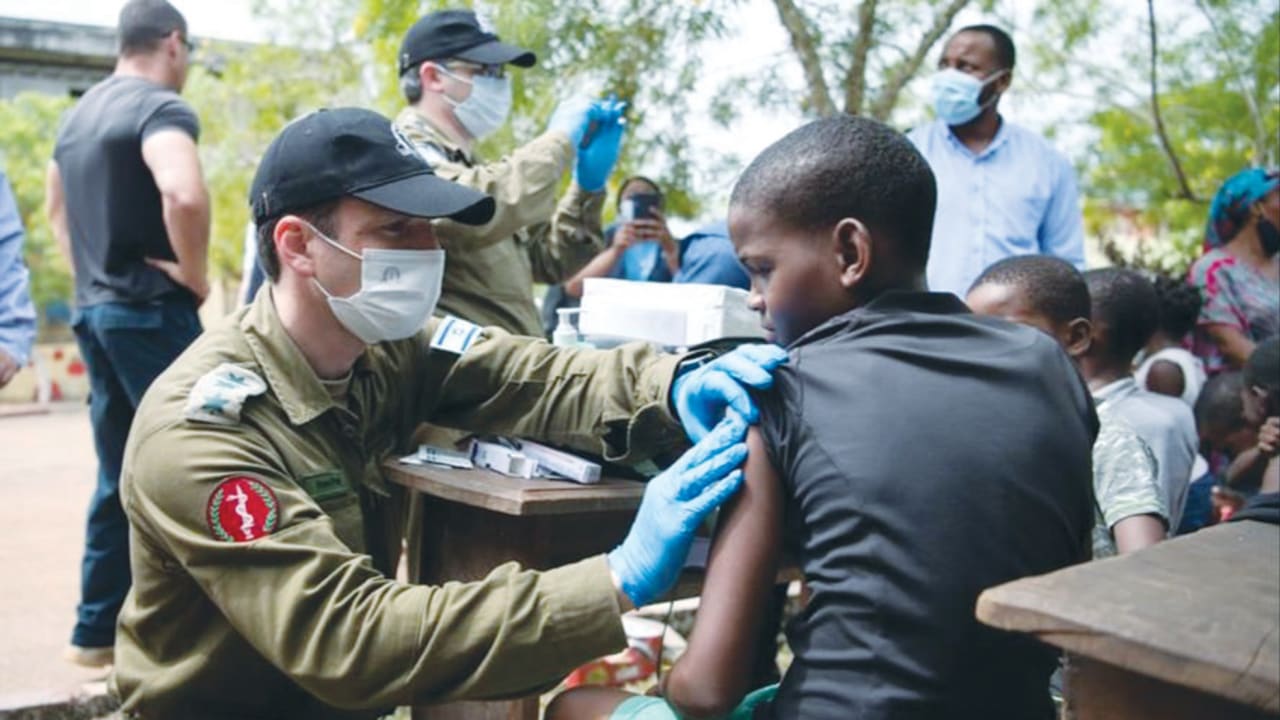
Outgoing IDF deputy chief medical officer Noam Fink feels bound to help suffering civilians not just in Israel
Events in Israel and around the world have taken the deputy chief medical officer of the IDF – who normally worries about the health of soldiers and officers on the battlefield and in their daily activities – as far as Equatorial Guinea and as close as the border with Syria to help unfortunate civilians caught in a long civil war.
Col. Dr. Noam Fink, 47, has just concluded three-and-a-half years as deputy chief medical officer (surgeon-general) of the IDF Medical Corps. Previously, he served in a number of capacities in the military medical hierarchy.
He studied medicine at Tel Aviv University’s Sackler Medical Faculty in the Academic Atuda program, which enables high school graduates to defer their military service and go to the university first. Then he specialized in cardiology. After a year at Sheba Medical Center, he will compete with other physicians seeking to replace IDF Chief Medical Officer Prof. Elon Glassberg, who previously taught surgery at Bar-Ilan University’s Azrieli Faculty of Medicine in Safed, when he leaves his post.
<br>Operation Good Neighbor
OVER FOUR years ago, an injured Syrian came to Israel’s northern border asking for medical help from the IDF. Back then, there was no policy, just a commander’s on-the-spot decision to provide care to an injured civilian.

The aid to civilians in a country that is officially at war with Israel has continued on a near-daily basis.
In June 2016, as part of a decision to expand humanitarian aid efforts, the IDF Northern Command established the headquarters of Operation Good Neighbor, whose aim was to provide humanitarian aid to as many people as possible while maintaining Israel’s policy of noninvolvement in the conflict. The first activities coordinated by the headquarters took place the following month.
“Based on my 20-year medical career, I can truly say that the medical care we have provided to our neighbors here in the north of Israel is one of the most significant efforts to treat those in need that I have ever witnessed,” said Fink then, when he was chief medical officer of the Northern Command. “I deeply hope that our contribution will have a direct impact on the lives of our Syrian neighbors.”
About 200,000 residents of the Hauran region of southwestern Syria received help from Israel during the Syrian civil war, which began in March 2011 when security forces of Syrian President Bashar Assad opened fire on and killed several pro-democracy protesters in the southern Syrian city of Deraa. The uprising spread throughout the country, demanding Assad’s resignation and an end to his authoritarian leadership, and tapered off in 2018. More than 300,000 Syrian civilians died in the uprising.
“The people of Syria want peace with Israel,” one of the aid recipients wrote from an Israeli hospital. “To any Syrians that think that Israel is our enemy – you are wrong.”
Under Operation Good Neighbor, over 4,000 people were brought to Israel to receive treatment. A third of the recipients of Israeli aid were displaced persons or refugees, and half of them under the age of 18. The IDF also transferred medicine, supplies and equipment to Syrians across the border. An internationally managed field hospital was established at an Israeli outpost near the border.
Some 450,000 liters of fuel were transferred for heating, operating water wells and ovens in bakeries. The IDF also transferred seven generators, water pipes to rebuild Syrian infrastructure, and equipment for a temporary school in the region. The IDF also sent 40 tons of flour to bakeries, 225 tons of food, 12,000 packages of baby formula, 1,800 packages of diapers, 12 tons of shoes and 55 tons of cold-weather clothing.
The IDF provided aid to Syrians on the other side of the border for two primary reasons, said Fink. “First, we have a moral imperative. We can’t stand by watching a severe humanitarian crisis without helping the innocent people stuck in the middle of the conflict. We also believe that the aid will ultimately create a less hostile environment across the border – and that will lead to improved Israeli security.”
“Based on my 20-year medical career, I can truly say that the medical care we have provided to our neighbors here in the north of Israel is one of the most significant efforts to treat those in need that I have ever witnessed.”
Dr. Noam Fink
<br>IDF vs the COVID-19 pandemic
NOT LONG after Fink began his job as deputy chief medical officer, the world, Israel and the IDF were hit by the COVID-19 pandemic. Many soldiers of all ranks were infected, and military training and ongoing activities were disrupted. Fink was the IDF’s corona project manager, charged with ensuring vaccinations, enforcement of mask wearing, testing, isolation of those infected using a mobile laboratory, canceling leaves for soldiers, transitioning to capsules and other policies to prevent the further spread of the virus.
“At the beginning of the first wave, we had the ability to conduct 300 corona tests a day. Today, we can conduct 1,000 a day, and soon we will have the capability to conduct up to 2,000 tests a day,” said Fink during the first year of the pandemic.
The IDF also provided a hotline which soldiers can turn to with questions about the pandemic, or to schedule a test.
“I am not sure we won’t have another wave – a seventh – of COVID-19 in the winter,” Fink told The Jerusalem Post in an interview initiated by the IDF Spokesman’s Office before the conclusion of his service as deputy chief medical officer.
“We offered soldiers three Pfizer vaccinations. It was not mandatory, but about 90% agreed to roll up their sleeves. But now the efficacy of the vaccinations has been reduced, as so much time has passed. We may have to offer the same vaccines again to increase immunity. No new vaccines suited to the latest variants have yet been approved by the US Food and Drug Administration [FDA] and put on the market.”
The Medical Corps is also preparing to cope with influenza. According to reports in the southern hemisphere, where the winter is ending, the flu is expected to be tough here in our winter. All soldiers willing to get vaccinated will be able to get a shot, Fink promised. “Since many soldiers are in close quarters, the virus spreads easily.”
“I am not sure we won’t have another wave – a seventh – of COVID-19 in the winter."
Dr. Noam Fink
Knights of Equatorial Guinea
LAST YEAR, the IDF sent a humanitarian aid delegation to the Republic of Equatorial Guinea on the west coast of Central Africa which brought with it two tons of medical equipment. The IDF team included 55 doctors, nurses and paramedics from the Medical Corps and nine representatives of the Rescue and Training Division, including engineers and civilian assistance specialists in both regular and reserve service.
As a token of appreciation for the delegation’s activities, Guinea’s president presented it with the Medal of Honor, “Knight of Equatorial Guinea.”
During the delegation’s seven days of operation, medical forces worked in the three hospitals in the city and operated mobile clinics for villages on the outskirts, providing medical assistance to 725 patients, and performing 92 lifesaving surgeries and medical procedures.
“The aid delegation has fulfilled its mission – saving lives. We were proud to stand by our ally Equatorial Guinea and represent the State of Israel.”
Dr. Noam Fink
At the same time, the rescue and training forces surveyed dangerous structures.
The delegation, under Fink’s command, formulated professional recommendations for improving the medical response in the city by building medical institutions and upgrading them. In addition, the delegation trained staff at the three local hospitals to deal with multi-casualty incidents. The delegation led the coordination with other foreign missions in Equatorial Guinea and international aid organizations, including the World Health Organization and the United Nations Office for the Coordination of Humanitarian Affairs.
“The aid delegation has fulfilled its mission – saving lives. We were proud to stand by our ally Equatorial Guinea and represent the State of Israel,” Fink declared.
<br><br>Battlefield medicine
BUT THE cardiologist said that his “first hat is medicine on the battlefield, special campaigns and ongoing medicine for combat soldiers. We cooperate with the US Army, and we are more flexible because Israel doesn’t have an institution like the FDA.”
Fink has maintained contact with the US, British, German, Spanish and Australian military medical corps.
“They learn from us, and we learn from them. Soon, at the end of September, will be a conference in Washington, DC, that we hold with our US counterparts. It rotates between Israel and the US every year; our strongest cooperation is with the Americans. We will send dozens of representatives to the conference,” Fink said.
In the US military, it takes a decade to introduce new things, he asserted. “The IDF Medical Corps was the first in the world to use freeze-dried plasma made in Germany on the battlefield, and it has saved lives. We are able to make such a product ourselves, but because we need just hundreds of units a year, it is not an economic proposition.”
Since Operation Protective Edge against Hamas and other terrorist organizations in 2014, the freeze-dried plasma has been carried by every IDF doctor and paramedic.
“It was difficult during the height of the pandemic because civilians who used to donate [blood] in shopping centers could [no longer do so]. Soldiers had to make up the difference.”
Dr. Noam Fink
“We saved many lives with it. Before, we were able to give soldiers who lost blood only saline [salt] solution to raise their blood pressure,” explained Fink. “It is a standard of care. Red blood cells can’t be freeze dried, because they explode, and when only hemoglobin is given, it affects the clotting mechanism. Every IDF medic has a tourniquet to stop bleeding. There is even an American product called CAT that the wounded soldier can use on himself.”
Two-fifths of all donated blood in Israel is given to Magen David Adom by the IDF, whose soldiers volunteer to donate. “It was difficult during the height of the pandemic because civilians who used to donate in shopping centers could [no longer do so]. Soldiers had to make up the difference.”
As for chronic diseases like obesity and smoking-related conditions, which affect large numbers of Israeli civilians, Fink said more can be done to prevent them from affecting IDF personnel.
Menus in IDF cafeterias have improved and become more healthful, he said, but he concedes that while smoking is forbidden except in special “smoking corners,” he is aware of the fact that many young solders smoke cigarettes and vape electronic cigarettes. “There are sanctions against violators. We put special emphasis on preventing diseases in combat soldiers on active duty, who are fed five or six times a day, including a lot of protein, because of the energy they expend.”
But what about the routine medical care of officers and soldiers at Tel Aviv’s Kirya military headquarters and other places where noncombatants work, day in and day out? Many there have been complaining for years about a severe shortage of physicians and dentists, having to wait for months to see a family physician or specialist at the clinics there or being forced to travel long distances to bases in the North or South to get treatment, and even then having to wait for months for an appointment.
Several years ago, the Medical Corps announced that it was arranging with the four public health funds to offer ongoing medical care to soldiers, who are not permitted to join them and who are dependent on inadequate IDF medical services. In many cases, soldiers – including pregnant women – have paid private doctors to get urgent care. But then the program to incorporate the public health funds was canceled without explanation, apparently because the health maintenance organizations demanded a high price for the service.
“We are aware of the challenges and the queues for care,” said Fink.
At the beginning of August, the IDF unveiled a new program, Health for You, to “revolutionize” military healthcare. In an attempt to reduce waiting times for medical appointments and improve overall, the IDF said it was moving more toward digitization while adding more clinics and manpower. The changes to the Medical Corps by the IDF’s Technological and Logistics Directorate were said to be part of an “extensive program to improve and reform several issues in the army that affect the well-being of troops.” The corps claimed there would be additional new clinics and renovated existing ones, and more doctors and dentists, especially in the Arava and the West Bank.
But many soldiers have their doubts that the situation will be better.
“It is a skeptical generation,” concluded Fink. “There are things we have to improve, and some have already begun. It is a three-year program, and better medical services will be evident already next year.”
The IDF Spokesman’s Office promised to arrange for a Post interview with Dr. Erez Karp, who is directly responsible for ongoing medical care for non-combat soldiers, in the near future.