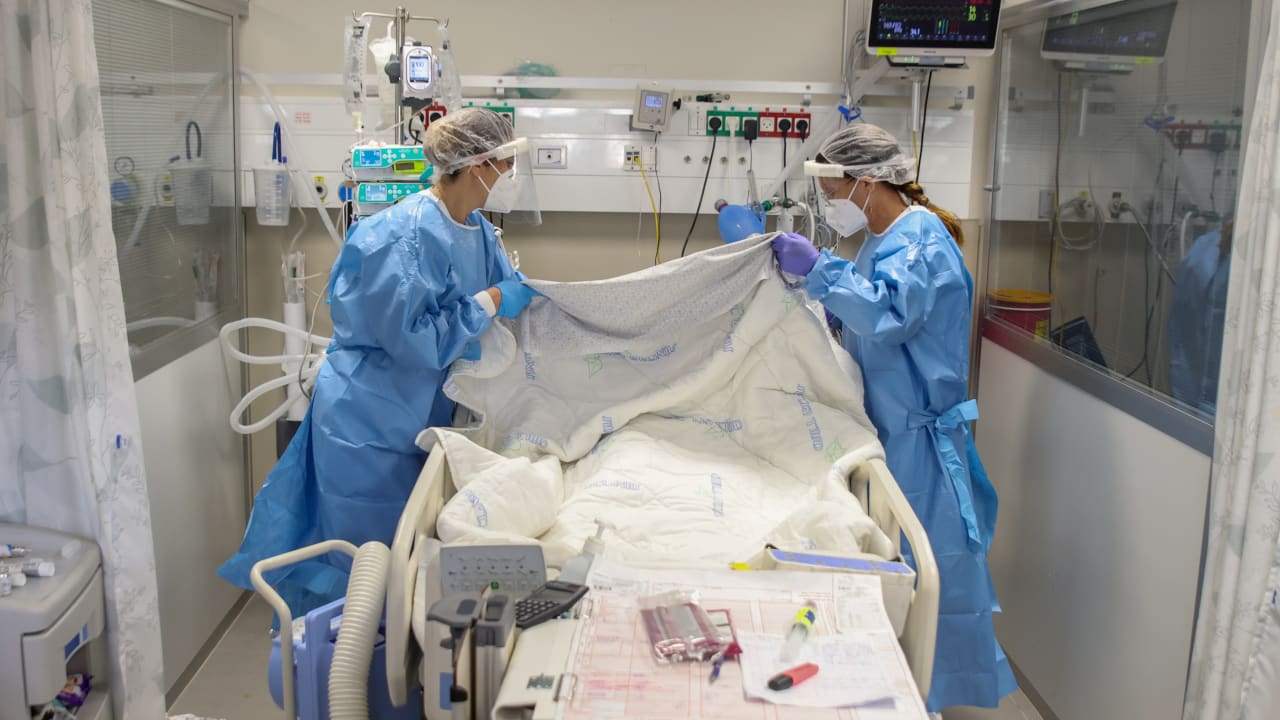
Doctors are being asked to play God less than 10 days after Yom Kippur.
The country’s hospitals are overcrowded. Their coronavirus wards are collapsing and the doctors who are trying to treat all of these patients are crashing. There is not enough lifesaving equipment, nor skilled personnel to manage it.
We read in the U’Netaneh Tokef prayer: “How many will pass from the earth and how many will be created? … Who will die at his predestined time and who before his time… who by famine, who by thirst … who by plague?”
Will Israeli doctors be the ones to decide?
“We are very close to a situation of choosing among patients” in the coronavirus wards, said Dr. Masad Barhoum, the director of Galilee Medical Center this week.
A 53-year-old man was hospitalized in serious condition, but not from coronavirus, in a relatively small hospital that did not have any ECMO machines. He died while the hospital was trying for too long to find a larger medical center that could treat him, N12 reported.
The majority (about 40) of the country’s “heart-lung machines” are being used by unvaccinated COVID-19 patients. According to hospital staff, when about six or seven more patients are put on ECMO machines, hospitals will be forced to turn away others who need them.
It is not just the number of devices, but also the manpower to manage them. Every patient on an ECMO machine requires 24/7 nursing care.
“We have no staff to deal with these people,” Dr. Yael Haviv-Yadid, the head of an intensive care unit and coronavirus ICU at Sheba Medical Center, told The Jerusalem Post. “We may always have spare machines, but we won’t have the staff to run them.”
While the Health and Finance ministries delivered additional funds to the hospitals to hire new staff, it did not all come and certainly not in time.
Junior doctors need to be trained, Haviv-Yadid explained.
Moreover, in the Arab sector, where there has been a 150% increase in serious patients, the medical aid organization Yad Sarah has said it has a shortage of portable oxygen tanks, which can help keep some COVID patients out of the overcrowded hospitals.
“With great pain, we are forced to turn away patients,” said Yad Sarah CEO Moshe Cohen. “We are begging for oxygen tanks in order to make room in the coronavirus wards and save lives.
There are also not enough hospital beds.
In the first COVID wave, the government instructed hospitals to refrain from offering any voluntary surgeries or treatments, shutting themselves off to nearly all but emergency and COVID patients. In subsequent waves, many people were still afraid to seek care at hospitals where they thought they might contract the virus.
Also, lockdowns kept people inside.
However, once the country resurfaced in the spring, doctors and hospitals saw an influx of patients, many who came in sicker and in need of greater care. The beds were full when the fourth wave began – even before the COVID patients started to arrive.
Now, doctors cannot put some ventilated COVID-19 patients into their hospitals’ dedicated coronavirus intensive care units where they belong, but instead have to leave them in coronavirus internal medicine wards where they will be cared for by less skilled and experienced nursing and other medical staff.
At Ziv Medical Center in Safed, Dr. Shimon Edelstein, who directs the hospital’s Unit for Infectious Diseases, said that the hospital is simply full. It has already started closing down units, from geriatric to neurology.
“We had to take the staff from these units to deal with the coronavirus patients,” Edelstein said. “This means we cannot do operations. It is not only a matter of saving lives, but also quality of life.”
Ziv does not have any ECMO machines, nor any staff trained to use them. That means that if patients require such care, they have to be transferred somewhere else.
On the evening of Yom Kippur, a medical team from Hadassah-University Medical Center had to travel all the way from Jerusalem to Safed (about 2 hours and 40 minutes) to urgently get and connect a 40-year-old to an ECMO machine before he died.
Between Haifa and Tel Aviv there are no ECMO machines, according to Dr. Mickey Dudkiewicz, director of Hillel Yaffe Medical in Hadera. With most machines in the center already taken, Edelstein said that the only option was Jerusalem.
The pressure is starting to crush the medical staff.
Ziv is a hospital with only 330 beds. Among them are 31 coronavirus patients, including 11 who are being treated in the ICU. But there are also patients in the regular ICU. The hospital only staffs four ICU experts, who Edelstein said are now being stretched too thin.
He said that the hospital lacks the specialists it needs, so the ones it has are being forced to run back and forth between departments.
“They work so hard, around the clock, and they have to endure all the suffering of these COVID patients and their families. It is very depressing and very tiring,” he said.
All while the numbers are not declining.
The Arab sector, where schools have been fully open, saw a 150% spike in serious morbidity in the last five weeks. A similar pattern, if nothing changes, can be expected when Jewish schools resume after Simhat Torah.
Haviv-Yadid said that most of the serious patients are under the age of 60 at this point and, at least at Sheba, none of them are vaccinated.
“I have one that is 30, 34, 35, 38, 50, 57 …” Haviv-Yadid recited. “I don’t think that someone who was not vaccinated deserves a death sentence. But if coronavirus patients are not treated this means death.”
This past month, an average of 23 people have died of COVID-19 each day.
“Each of those deceased has a name, a face and a broken and pained family,” said former Constitution, Law and Justice Committee Chairman MK Yakov Asher on Wednesday. “The prime ministers are transmitting to the public that the value of life is no longer above everything on the Israeli scale of values.”
The National COVID-19 Experts Committee warned the government on Thursday that its policy of relying on a third booster shot and minimal economic restrictions is not proving itself.
They too said that Israel, like other countries, is likely to be faced with the tragic dilemma of prioritizing young patients in need of critical care for coronavirus or otherwise over senior patients and called for a change in policy.
Without one, the government has silently issued a death decree - at least for those who have the misfortune to have fallen critically ill.