Circumventing the injection of an egg with sperm, Weizmann Institute of Science geneticists have accomplished a breakthrough – creating synthetic mouse embryos with beating hearts and brains outside the uterus using stem cells taken from skin and cultured in a dish.
“The embryo is the best organ-making machine and the best 3D bioprinter; we tried to emulate what it does,” noted research team head Prof. Jacob Hanna of the Molecular Genetics Department in the Rehovot institute.
Scientists already know how to restore mature cells to “stem-ness” – pioneers of this cellular reprogramming won a Nobel Prize in 2012. But going in the opposite direction – that is, causing stem cells to differentiate into specialized body cells, not to mention form entire organs – has proved much more problematic.
Why is it more problematic?
“Until now, in most studies, the specialized cells were often either hard to produce or aberrant, and they tended to form a mishmash instead of well-structured tissue suitable for transplantation,” he said. “We managed to overcome these hurdles by unleashing the self-organization potential encoded in the stem cells.”

"We managed to overcome these hurdles by unleashing the self-organization potential encoded in the stem cells."
Prof. Jacob Hanna
The breakthrough has just been published in the journal Cell under the title “Post-Gastrulation Synthetic Embryos Generated Ex Utero from Mouse Naïve ESCs.”
An egg meeting a sperm has always been the necessary first step in the beginning of sexually created life, and it’s also a common first step in embryonic development research. But Hanna’s team has done so without the use of fertilized eggs.
What does this mean for the future?
The method opens new horizons for studying how stem cells form various organs in the developing embryo and may one day make it possible to grow tissues and organs for transplantation using synthetic embryo models.
Hanna’s team built on two previous advances in his lab. One was an efficient method for reprogramming stem cells back to a naïve state – that is, to their earliest stage – when they have the greatest potential to specialize into different cell types.
The other, described in a scientific paper in Nature in March 2021, was the electronically controlled device the team had developed after seven years of trial and error for growing natural mouse embryos outside the womb.
The device keeps the embryos bathed in a nutrient solution inside of beakers that move continuously, simulating the way nutrients are supplied by maternal blood flow to the placenta, and closely controls oxygen exchange and atmospheric pressure. In the earlier research, the team had successfully used this device to grow natural mouse embryos from day five to day 11.
In the new study, the team set out to grow a synthetic embryo model solely from naïve mouse stem cells that had been cultured for years in a petri dish, without starting with a fertilized egg. This approach is extremely valuable because it could, to a large extent, bypass the technical and ethical issues involved in the use of natural embryos in research and biotechnology.
Even in the case of mice, certain experiments are currently unfeasible because they would require thousands of embryos, whereas access to models derived from mouse embryonic cells, which grow in lab incubators by the millions, is virtually unlimited.
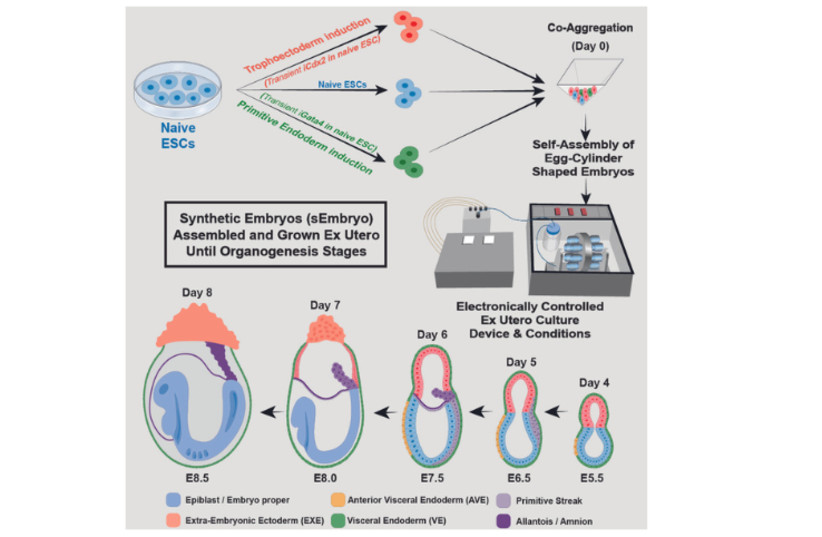
Before placing the stem cells into the device, the researchers separated them into three groups. In one, which contained cells intended to develop into embryonic organs themselves, the cells were left as they were. Cells in the other two groups were pretreated for only 48 hours to overexpress one of two types of genes – master regulators of either the placenta or the yolk sac. “We gave these two groups of cells a transient push to give rise to extraembryonic tissues that sustain the developing embryo,” Hanna explained.

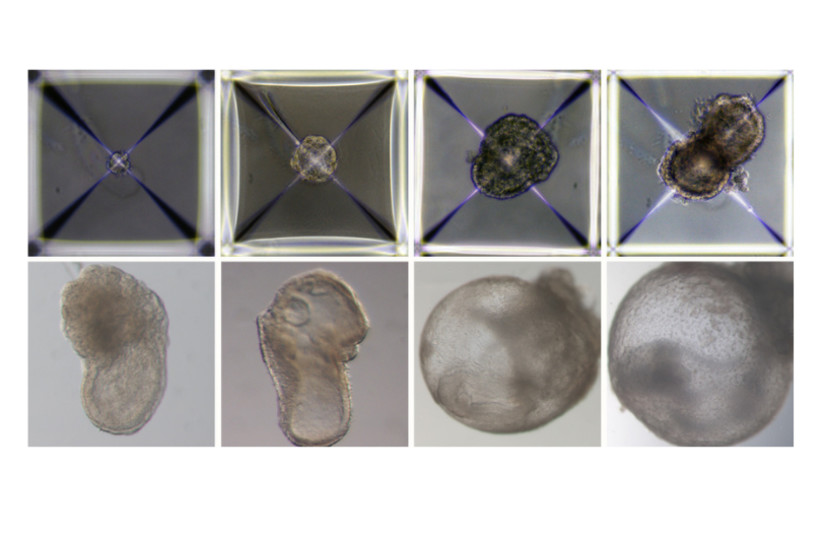
Soon after being mixed together inside the device, the three groups of cells convened into aggregates, the vast majority of which failed to develop properly. But 50 of around 10,000 went on to form spheres, each of which later became an elongated, embryo-like structure. Since the researchers had labeled each group of cells with a different color, they were able to observe the placenta and yolk sacs forming outside the embryos and the model’s development proceeding as in a natural embryo.
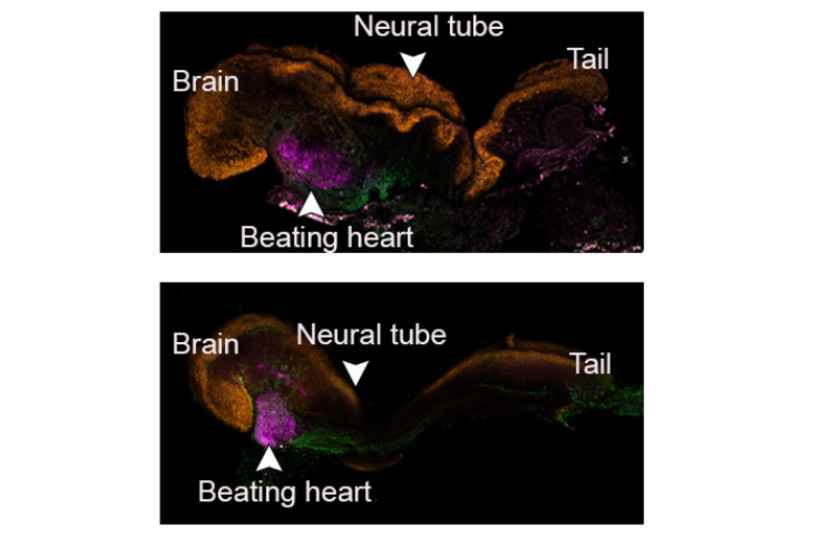
The synthetic models developed normally until day 8.5 – nearly half of the mouse 20-day gestation – at which stage all the early organ progenitors had formed, including a beating heart, blood stem cell circulation, a brain with well-shaped folds, a neural tube and an intestinal tract.
When compared to natural mouse embryos, the synthetic models displayed a 95% similarity in both the shape of internal structures and the gene expression patterns of different cell types. The organs seen in the models gave every indication of being functional.
For Hanna and other stem cell and embryonic development researchers, the study presents a new platform.
“Our next challenge is to understand how stem cells know what to do – how they self-assemble into organs and find their way to their assigned spots inside an embryo,” he said. “And because our system, unlike a womb, is transparent, it may prove useful for modeling birth and implantation defects of human embryos.”
Synthetic embryo models will not only minimize the use of animals in research, but they could also eventually become a reliable source of cells, tissues and organs for transplantation.
“Instead of developing a different protocol for growing each cell type – for example, those of the kidney or liver – we may one day be able to create a synthetic embryo-like model and then isolate the cells we need,” Hanna said. “We won’t need to dictate to the emerging organs how they must develop: The embryo itself does this best.”
"We may one day be able to create a synthetic embryo-like model and then isolate the cells we need. We won’t need to dictate to the emerging organs how they must develop. The embryo itself does this best."
Prof. Jacob Hanna
The research was co-led by Shadi Tarazi, Alejandro Aguilera-Castrejon and Carine Joubran of Weizmann’s Molecular Genetics Department.
Study participants also included Shahd Ashouokhi, Dr. Francesco Roncato, Emilie Wildschutz, Dr. Bernardo Oldak, Elidet Gomez-Cesar, Nir Livnat, Sergey Viukov, Dmitry Lokshtanov, Segev Naveh-Tassa, Max Rose and Dr. Noa Novershtern of the department; Montaser Haddad and Prof. Tsvee Lapidot of Weizmann’s Immunology and Regenerative Biology Department; Dr. Merav Kedmi of Weizmann’s Life Sciences Core Facilities Department; Dr. Hadas Keren-Shaul of the Nancy and Stephen Grand Israel National Center for Personalized Medicine; and doctors Nadir Ghanem, Suhair Hanna and Itay Maza of the Rambam Medical Center.
