A new magnetic resonance imaging (MRI) technology that non-invasively assesses iron levels in the human brain, shedding light on its critical role in brain function, aging, cancer, and neurodegenerative disorders has been developed by researchers at the Hebrew University of Jerusalem (HU), Tel Aviv Sourasky Medical Center, and Shaare Zedek Medical Center (SZMC).
People’s iron balance, determined by the milieu of available iron compounds, is impaired in aging, neurodegenerative diseases, and cancer, they wrote, but a non-invasive assessment of different molecular iron environments implicating brain tissue’s iron homeostasis (balance) remains a challenge. They say theirs is an innovative approach, based on quantitative MRI, distinguishes between healthy and pathological brain tissue without contrast agents, and provides insights into iron-related disorders, offering a significant advancement in neuroscience and healthcare.
The research team was led by Shir Filo and Prof. Aviv Mezer of HU, together with Dr. Tal Shahar, director of the neurosurgical oncology unit at Sourasky’s neurosurgery department. The study, “Non-invasive assessment of normal and impaired iron homeostasis in the brain,” has just been published in the journal Nature Communications.
The groundbreaking MRI technology promises to revolutionize scientists’ understanding of iron homeostasis in the human brain.
Traditional MRI scans provide qualitative images that require subjective interpretation by medical professionals, while quantitative MRI seeks to replicate the precision of assessing body temperature accurately and objectively when ill, moving beyond qualitative observations like “too hot” or “too cold.”
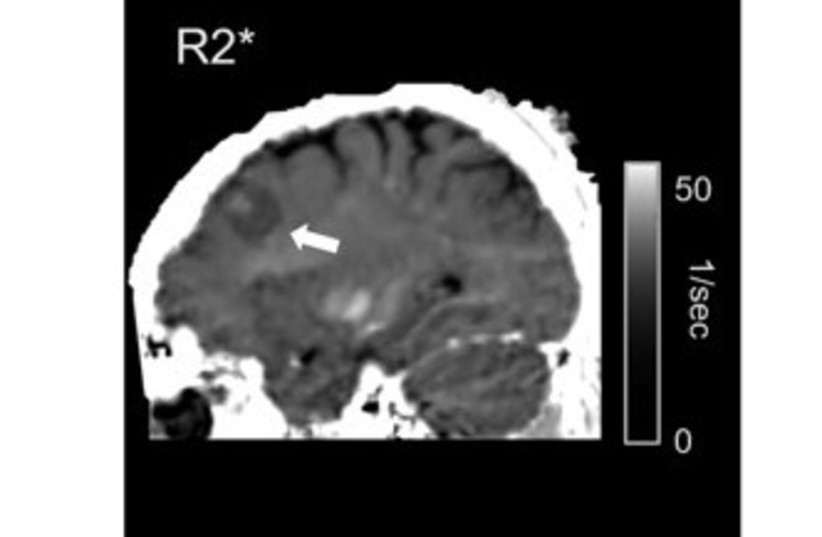
Maintaining the balance of iron
Achieving this requires intricate physical models that integrate multiple MRI scans to produce a diverse array of measurements. These MRI measurements are then leveraged to uncover valuable biological insights – like a blood test’s ability to reveal its composition, including proteins, fats, and potential irregularities.
One critical aspect of brain function is maintaining the balance of iron, which is vital for overall health. Imbalances in the brain’s iron levels have implications for various conditions, including neurodegenerative diseases and cancer. Until recently, the non-invasive assessment of the molecular iron environment within the living human brain posed a significant challenge.
The research team from the three institutions introduces a novel MRI approach based on quantitative MRI, which can sensitively detect changes in brain iron homeostasis. In their in-vitro (in a test tube or petri dish) experiments, the new technology revealed distinct paramagnetic properties of key iron compounds including ferritin, transferrin, and ferrous iron.
The real breakthrough came with in-vivo MRI scans of patients with brain tumors, operated at SZMC’s neurosurgery department, where the technology was also validated against ex-vivo iron compound quantification of the resected tumors. These ex-vivo transcriptomics and proteomics analyses were carried out in the lab of HU’s Dr. Naomi Habib, SZMC’s molecular neuro-oncology lab, which at the time of the study was directed by Shahar.
This innovative MRI approach demonstrates sensitivity to changes in iron mobilization capacity across different brain regions and during brain aging. It offers insights into changes in iron homeostasis and iron-related gene expression in pathological tissues. Most notably, it can differentiate between tumor tissue and non-pathological tissue without the need for the injection of toxic contrast agents.
“Our technology opens up new possibilities for understanding the role of iron in cancer, normal aging, and neurodegenerative diseases,” Filo explained.
“It enables non-invasive research and diagnosis of iron homeostasis in the living human brain, offering a potential game-changer for healthcare and neuroscience.”
Mezer stressed that “the strength of our team lies in its diverse composition, comprising experts from various disciplines and specialties. Dr. Shahar was leading the medical aspect of the study involving meningioma patients and proteomic studies. Dr. Rona Shahrabani was instrumental in conducting experiments with iron proteins, while Dr. Nevo Margalit, head of SZMC’s neurosurgery department, made a substantial contribution through his involvement in a significant portion of the surgeries and recruitment of patients,” he added.
“Additionally, SZMC radiologist Dr. Eli Ben David played an indispensable role in enabling the MRI scans and Dr. Habib brought the valuable knowledge in gene expression. Their collective and truly interdisciplinary expertise and unwavering dedication significantly enhanced the success of this pioneering study,” Mezer concluded.
